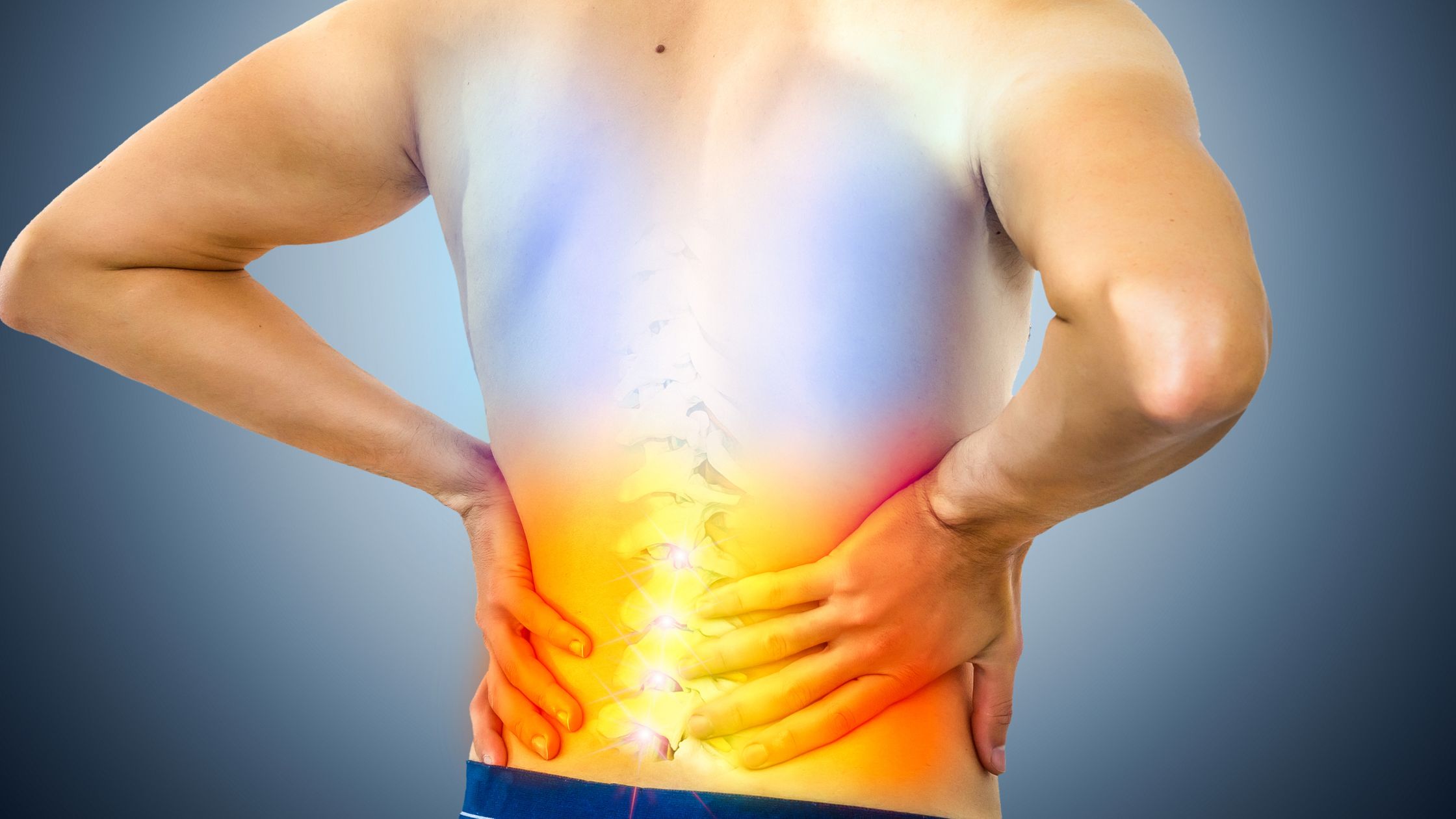
Back pain is common. Sciatica is also common. But just because they’re common doesn’t mean they’re not dangerous. For most people, sciatica starts as back pain that moves into the buttock and down the leg. It may feel sharp, burning, electric, or numb.
Often, it improves with time, movement, medication, and physical therapy. But some cases are different. Certain symptoms can indicate the nerve is seriously compressed, not just irritated. When that happens, taking too long to find treatment brings risks of lasting weakness, numbness, or permanent loss of bladder and bowel function.
The key is knowing the difference between a painful flare-up that can be managed and a true spine emergency. When you understand the signs of severe sciatica that require immediate attention, you have a better chance of protecting your mobility and long-term nerve function.
Quick Answer: When should you see a spine surgeon for sciatica?
What are the red flags for sciatica?
The main red flags for sciatica are progressive leg weakness, foot drop, numbness in the groin or inner thighs, and any new loss of bladder or bowel control. These symptoms can point to severe nerve compression and may need urgent treatment.
When is sciatica an emergency?
Sciatica is an emergency when it moves from just pain to loss of function. That includes sudden or worsening leg weakness, cauda equina syndrome symptoms, saddle numbness, or changes in bladder or bowel control. If any of those happen, you should seek emergency medical care right away.
When should you see a spine surgeon for sciatica?
You should see a spine specialist if your sciatica lasts longer than about six weeks, keeps getting worse, or starts causing weakness instead of pain alone. You should get emergency care right away if you develop foot drop, numbness in the groin or inner thighs, or any new trouble controlling your bladder or bowels. Those symptoms can point to severe nerve compression or cauda equina syndrome, which needs urgent evaluation.
Why are cauda equina syndrome symptoms so serious?
Cauda equina syndrome symptoms are serious because they can signal severe compression of the nerve bundle at the base of the spinal canal. Without urgent evaluation and treatment, that pressure can lead to permanent weakness, numbness, or loss of bladder and bowel function.
What Is Sciatica?
The term “sciatica” describes a pattern of symptoms, not a single diagnosis. It describes pain that travels along the sciatic nerve pathway, usually from the low back into the buttock and down the leg. It might feel like burning pain, tingling, numbness, or weakness, most often only on one side. Coughing, sneezing, or sitting for long periods can make it worse.
The most common cause is a herniated lumbar disc pressing on a nerve root. Other causes include spinal stenosis, spondylolisthesis, and, less commonly, infection, tumor, or trauma. In short, sciatica is the body’s way of telling you that a spinal nerve is irritated or compressed. For a broader explanation of the condition itself, see what is sciatica.
When Sciatica Is Usually Not an Emergency
Most sciatica does not need surgery. In fact, the American Association of Neurological Surgeons notes that symptoms from herniated discs improve in about 9 out of 10 people, often within days to a few weeks. Mayo Clinic corroborates those findings. Mild sciatica often improves over time, especially with activity changes and self-care.
That is why early treatment usually focuses on:
- staying mobile rather than strict bed rest
- anti-inflammatory medication, when appropriate
- physical therapy
- posture and activity changes
- targeted injections in selected cases
This is the part many patients need to hear: pain alone, even intense pain, does not automatically mean you need an operation. Severity matters, but function matters more. If you’re still trying to manage symptoms conservatively, you may also want to review how to get sciatica relief.
The 6-Week Guideline: When Persistent Sciatica Needs a Specialist
The six-week mark is an important threshold in sciatica care. Most providers won’t recommend imaging unless symptoms have persisted for six weeks. Referrals to spine specialists are rare before four weeks. But that doesn’t mean you have to wait if you’re getting worse. It just means persistent symptoms are necessitating deeper evaluation. The problem may not resolve on its own.
If your pain is still strong after six weeks, or if it keeps interrupting sleep, walking, work, or basic daily tasks, it’s time to move beyond “let’s just give it more time.” At that stage, a specialist usually wants imaging, often an MRI, to find the exact level and cause of nerve compression. Nighttime symptoms can be especially disruptive, and patients often overlook hidden causes of sciatica pain at night that may point to worsening irritation.
Red Flag 1: Progressive Leg Weakness or Foot Drop
Pain is what clues you in, but weakness is what determines urgency. If your leg feels like it is giving out, if climbing stairs becomes harder, or if you cannot lift the front of your foot normally, (foot drop) that’s a red flag. Foot drop is especially concerning because it suggests the nerve is losing the ability to send signals to the muscles that lift the foot.
Sudden numbness or muscle weakness in a leg as a reason to get immediate medical care. Significant leg weakness often needs urgent evaluation and imaging. Patients often make the mistake of saying, “It’s just pain.” Weakness is not just pain. Weakness means function is being threatened.
Red Flag 2: Saddle Numbness
Numbness in the groin, inner thighs, buttocks, or around the anus is never something to “watch for a few days.” This is called saddle anesthesia, because it affects the areas that would contact a horse’s saddle. They’re harbingers of a very serious condition called cauda equina syndrome, where the nerves at the base of your spine are compressed. Cauda equina syndrome is a much more central and dangerous level of nerve compression.
Red Flag 3: Bladder or Bowel Changes
This is the symptom category patients should never try to self-manage. New trouble starting urination, urinary retention, leaking urine, fecal incontinence, or loss of normal awareness of bladder or bowel function can also signal cauda equina syndrome. Most healthcare providers consider this a medical emergency, and quick surgical treatment can prevent complications. Emergency decompression may be needed because the longer it goes untreated, the greater the chance of permanent paralysis and incontinence.
If you develop these symptoms, do not call for a routine office visit. Go to the emergency room.
When to Go to the Emergency Room for Sciatica
Go immediately if your sciatica comes with:
- new bladder or bowel problems
- numbness in the saddle area
- sudden or worsening leg weakness
- difficulty walking because of weakness or numbness
- severe symptoms after trauma
- back pain plus fever or signs of infection
These are some of the clearest signs of severe sciatica and answer the question of when sciatica is an emergency. They take the situation from “annoying pain” to “protect nerve function now”.
What a Neurosurgeon Looks For
A neurosurgeon does more than just decide whether you need surgery. They’re trying to answer a much more precise question: Is the nerve still irritated, or is it being injured?
That distinction shapes everything. A specialist will look at:
- strength testing
- walking pattern
- reflex changes
- sensory loss
- imaging findings
- progression over time
Symptoms that are just painful and not getting worse keep conservative care on the table. When they progress into weakness, numbness or dangerous patterns, or bladder and bowel dysfunction, the risk level increases.
Conservative Care vs Surgery for Sciatica
A balanced sciatica treatment plan is usually stepwise.
Phase 1: Early conservative care
During the first several weeks, treatment may include:
- activity modification
- walking and movement
- physical therapy
- anti-inflammatory medication
- selected injections
Phase 2: Imaging and specialist evaluation
If pain persists, worsens, or function declines, MRI or CT helps pinpoint where the nerve is compressed.
Phase 3: Surgical decision-making
Surgery enters the picture when:
- symptoms fail to improve after a reasonable trial of conservative treatment
- weakness is progressing
- function is dropping
- red flag emergency symptoms appear
Procedures such as microdiscectomy or decompression are designed to take pressure off the nerve. The goal is preserving or restoring function, not just relieving pain. Many patients also benefit from identifying common triggers for sciatica and what to do about them earlier in the process so they can avoid aggravating an already compressed nerve.
Key Takeaways: Your Sciatica Safety Checklist
- Most sciatica improves without surgery, often within days to several weeks.
- Pain that lasts beyond six weeks deserves a specialist evaluation.
- Progressive weakness, especially foot drop, is urgent.
- Saddle numbness is a major red flag.
- New bladder or bowel symptoms are an emergency.
- Cauda equina syndrome should be treated as a time-sensitive surgical condition.
Reclaiming Your Mobility Before the Damage Becomes Permanent
Sciatica is common, but you can’t get complacent with it.
The difference between a temporary flare and a neurosurgical emergency often comes down to weakness, numbness pattern, and bladder or bowel function. If your symptoms are lasting longer than six weeks, that’s a sign to escalate your evaluation. If you have foot drop, saddle numbness, or any bowel or bladder change, that is not the time to wait for the next opening on the calendar. It’s time to act.
The good news is that many patients do recover well, especially when the right intervention happens at the right time. The most important step is recognizing when your leg pain has crossed the line from miserable to urgent.
Resources
Cauda Equina Syndrome – Cleveland Clinic
Herniated Disc – American Association of Neurological Surgeons
Mensah EO, Chalif JI, Baker JG, Chalif E, Biundo J, Groff MW. Challenges in Contemporary Spine Surgery: A Comprehensive Review of Surgical, Technological, and Patient-Specific Issues. J Clin Med. 2024;13(18):5460. Published 2024 Sep 14. doi:10.3390/jcm13185460
Sciatica – Mayo Clinic